A Cost-Effective Solution for Safe Motherhood in Kenya
Many women do not receive adequate maternal health care due to the high-cost of services, which can result in financial catastrophe for uninsured, low-income families around the world. As of 2005, the World Health Organization estimated that 44 million households spent over 40% of their expendable earnings on health care, ultimately forcing 25 million families into poverty. 1 Health care financing through a subsidized voucher program is one possible solution to address this issue. However, the effectiveness of vouchers in actually reducing costs for individuals depends on the following: 1) whether service and transportation costs are subsidized, 2) the degree of service availability, and 3) community perceptions about the quality of care. Focusing on financial burden, a recent study examined the effects of a reproductive health vouchers program on out-of-pocket expenses for family planning, antenatal, delivery and postnatal care services in Kenya. 2
Health care Spending in Kenya
Over the past decade, government spending on health care in Kenya has remained consistently lower than that of neighboring countries. As a result, out-of-pocket spending is the largest source of payment for health care services. From 1996-1999, individual payments comprised 42%-48% of total health care expenditures. This financial burden is catastrophic for 5% of Kenyan households and even drives roughly 1.5 million people into poverty annually. 3
Reproductive Health Vouchers Program
The Kenyan government implemented the reproductive health vouchers program in efforts to reduce maternal and infant deaths by increasing the rates of childbirth in health facilities and improving access to health services. Essentially, by subsidizing the cost of reproductive health care, the poor are incentivized to use those services. The program consists of three components: 1) safe motherhood (focuses on pregnancy and childbirth), 2) long-term family planning, and 3) gender-based violence recovery services. Firstly, the safe motherhood voucher covers four antenatal care visits, delivery care (e.g. Caesarean section), postnatal care within six-weeks, and treatment of neonatal complications. Secondly, the family planning voucher covers long-term prevention, such as implants, intrauterine contraceptive device (IUCD), and surgical contraception. Thirdly, is a gender-based violence recovery services voucher (available to all women). Since 2006, the program is being rolled out to various communities over time.
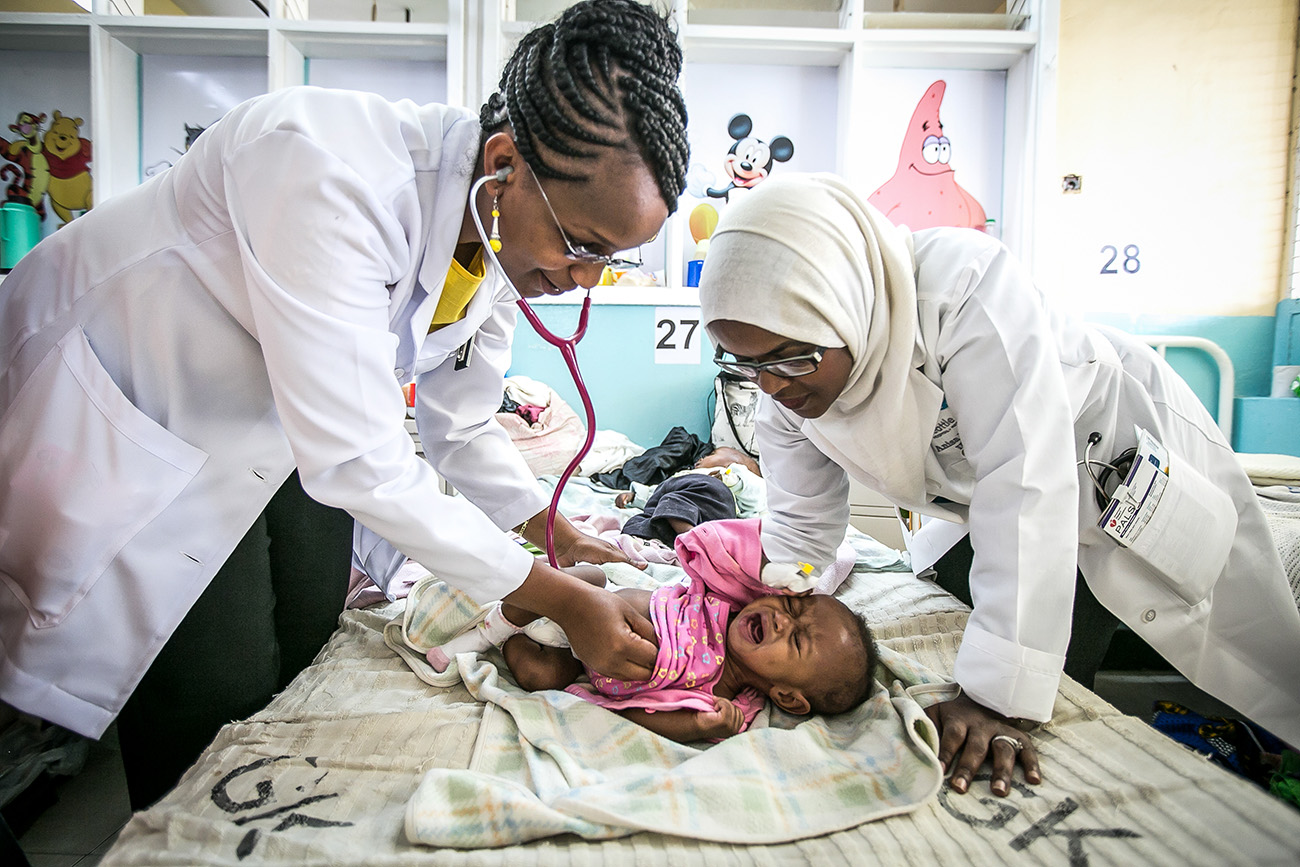
Photo: Global Health Photo
Methods
To examine the impact of the vouchers program, two rounds of surveys were administered to neighboring counties with similar population characteristics and available health facilities.
However, one county received vouchers while the other did not. Surveys were completed from May 2010 to July 2011 by 2,933 women aged 15-49 years, and from July to October 2012 by 3,094 women of similar ages. Statistical analyses (e.g. multivariate linear regression) were then conducted to assess the difference in out-of-pocket expenses and rates of care among voucher and non-voucher communities.
Results
Use of reproductive health services
Vouchers → more women received maternal health care
Over time, more women used the safe motherhood voucher when available. This increased from 15% to 44% by 2012. These women also used private health facilities at a much higher rate than women without vouchers. However, the use of family planning vouchers did not significantly change over time, as the number of women who paid for those services remained the same.
Changes in payment for services
Vouchers → less women paid out of pocket for safe motherhood services
Women from voucher sites paid significantly less for antenatal, delivery and postnatal care services than those from non-voucher sites. While vouchers contributed to less women paying for family planning, the greatest change was related to safe motherhood services.
Table 1. The average amount paid for health services (2010 – 2012) among voucher versus non-voucher sites.
| Voucher Sites | Non-Voucher Sites | ||
| Family Planning | No change | 52% Increase | |
| Safe Motherhood | Antenatal Care | 20% Decline | 78% Increase |
| Delivery Care | 52% Decline | 16% Decline | |
| Postnatal Care | 90% Decline | 40% Decline | |
Implications
The findings of this study suggest that increasing the use of vouchers will result in significant cost savings for women who receive reproductive health services. Marketing campaigns and increasing the number of health facilities offering vouchers can help achieve this goal. Ultimately, providing financial assistance and access to health care can protect the most vulnerable individuals from being forced into poverty.
..
Photo: University of Washington, School of Public Health
References:
1. World Health Organization (WHO). Designing health financing systems to reduce catastrophic health expenditure. Technical Briefs for Policy Makers No. 2. Geneva: WHO; 2005.
2. Obare, F, Warren, C, Kanya, L, Abuya, T, and Bellows, B. Community-level effect of the reproductive health vouchers program on out-of-pocket spending on family planning and safe motherhood services in Kenya. BMC Health Serv Res. 2015; 15: 343.
3. Chuma J, Maina T. Catastrophic healthcare spending and impoverishment in Kenya. BMC Health Serv Res. 2012;12:413.
4. Featured image: UNFPA






